The TDP-led coalition government’s budget allocations for drugs at major government hospitals in Andhra Pradesh for 2026-27 tell a story that is stark in its simplicity and devastating in its implications. Every major hospital in the state has seen its drug budget slashed, not trimmed, not adjusted, but slashed by between 35% and over 50% compared to the previous year.
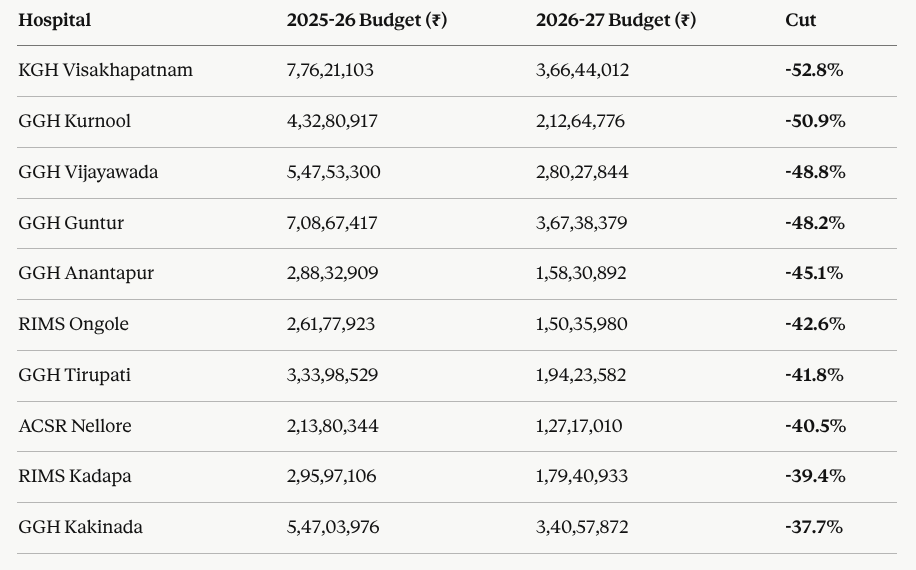
KGH Visakhapatnam one of the largest and most critical public hospitals in the state, serving a vast coastal and tribal population, has seen its drug budget cut by more than half. From ₹7.76 crore to ₹3.66 crore. GGH Kurnool, serving one of Andhra Pradesh’s most drought-prone and economically vulnerable districts, has had its budget cut by 50.9%. GGH Vijayawada, the hospital at the heart of the state’s administrative capital region by 48.8%.
To understand what a 52.8% cut to KGH Visakhapatnam’s drug budget actually means, it helps to think in terms of what ₹4.09 crore the amount cut from that hospital’s allocation buys in a hospital that serves thousands of patients every month.
It buys antibiotics for patients with infections who cannot afford private pharmacies. It buys insulin for diabetic patients who depend on the government supply. It buys blood pressure medications, anticoagulants, chemotherapy drugs, antiretrovirals, and the dozens of other medicines that keep chronic patients alive and functional. It buys the consumables — syringes, cannulas, IV fluids, wound dressings — without which basic medical procedures cannot be performed.
When ₹4.09 crore disappears from a hospital’s drug budget, it does not disappear as an abstraction. It disappears as medicine that is not on the shelf when a patient needs it. It disappears as a prescription that a doctor writes, knowing it cannot be filled. It disappears as a treatment that is delayed, diluted, or denied.
These are not marginal reductions in a time of fiscal prudence. These are cuts that healthcare professionals, hospital administrators, and doctors themselves have described as incompatible with delivering basic patient care.
Beyond Medicine: The Collapse of Diagnostics
The crisis is not confined to medicines. Across multiple hospitals in Andhra Pradesh, diagnostic services the fundamental tools through which doctors understand what is wrong with their patients, are breaking down.
Patients at some hospitals are now being asked to pay for X-ray films and other consumables. In a government hospital that exists specifically to provide free healthcare to people who cannot afford private facilities, asking a patient to pay for an X-ray film is not an inconvenience. It is a policy failure wearing the face of a broken promise.
CT scan services, which are critical for neurological emergencies, cancer diagnosis, internal trauma assessment, and dozens of other conditions, are reported to be irregular across the state. For a patient arriving at a government hospital with a suspected brain bleed or internal injury, an irregular CT scan service is not a minor inconvenience. It is a threat to their survival.
The 175 community health centres that serve Andhra Pradesh’s rural population, the first point of institutional healthcare contact for millions of people in villages and mandals across the state are facing the same squeeze. Their drug allocations, their diagnostic capacity, and their ability to function as functional healthcare nodes rather than empty buildings with government boards are all under pressure from the same budgetary axe.
Arogyasri Neglected:
Under Jagan Mohan Reddy’s government, Aarogyasri was expanded, strengthened, and positioned as the primary healthcare safety net for Andhra Pradesh’s poor covering treatments at network hospitals, ensuring that a family facing a medical emergency did not also face financial ruin.
The TDP government’s relationship with Aarogyasri has been troubled. Due to the network hospitals mounted. Hospitals began refusing to treat Aarogyasri patients. The scheme that was supposed to be the bridge between poor patients and quality healthcare became increasingly unreliable.
Now, with government hospital drug budgets cut by up to 52.8%, the two pillars of public healthcare for Andhra Pradesh’s poor are simultaneously weakening. Government hospitals are running out of medicines. The insurance scheme meant to fund treatment at private network hospitals is not functioning as designed. The poor patient in Kurnool, in Visakhapatnam, in Anantapur, in Kakinada has no reliable path to care.
The drug budget cuts are the latest chapter in a pattern of healthcare neglect that has been documented across Andhra Pradesh under the current government. Recently, a newborn died at a government hospital in circumstances involving failures of power supply, oxygen availability, and institutional accountability. No power. No oxygen. No accountability. A newborn’s life, ended by the compounding of institutional failures that each, individually, might have been manageable but together proved fatal.
This is what healthcare neglect looks like at its most acute. Not the abstract language of budget percentages but the concrete reality of a family that brought a child into a government hospital expecting care, and left without one.
Healthcare in Crisis :
This crisis does not happen in a vacuum. The TDP government came to power in 2024 promising development, investment, and the Amaravati capital city dream. Its fiscal priorities have been shaped by the enormous financial commitments those promises entail, infrastructure projects, capital development, and the Swarnandhra vision.
Somewhere in the allocation of a constrained budget, healthcare for the poor was deprioritised. The drug budgets at government hospitals were cut in half. The community health centres serving rural populations were squeezed. The diagnostic services that poor patients depend on were allowed to deteriorate.
This is a political choice. Budgets are political documents. They express priorities. And the 2026-27 budget of the TDP government expresses, in rupees and percentages, a priority ordering in which major government hospitals in Andhra Pradesh can function on half their drug allocation.
Healthcare professionals across the state are saying clearly that this is not sustainable. The ten-day medicine shelf in Anantapur is not a warning for the future. It is a present crisis.
This is not a healthcare system under pressure. This is a healthcare system being systematically defunded while the people it exists to serve the poor, the rural, the vulnerable, have nowhere else to turn. The TDP government has issued a prescription for neglect and the poor of Andhra Pradesh are the ones paying the price.



